Chapter 21: Characteristics of Employee Benefits
Overview: This chapter examines both the required benefits that employers must provide, including Social Security, unemployment insurance and Workers' Compensation, as well as the discretionary employer-provided benefits, such as retirement plans, insurance programs and time off.
Corresponding courses
20 The Basics of Equity Compensation
50 Employee Life and Disability Insurance
INTRODUCTION
Employee benefits consist of a large number of diverse organizational reward offerings. This diversity makes it difficult to categorize and discuss the characteristics of benefits in general, since each one needs to be dealt with independently. In fact, benefits administration has become a specialized function within organizations that requires specific training and experience.1 This field is changing so rapidly that there will undoubtedly be further changes by the time that you read this material.
CONSIDERATIONS IN BENEFIT ANALYSES
Although it is hard to distinguish commonalities among benefits, there are a number of factors that need to be considered when discussing any benefit. Those to be examined briefly here are purpose, legal requirements, contributions, and cost.
Purpose
The central purpose of benefits in the employment exchange is to foster membership and continuity of employment. From the employee's perspective security is a major theme in benefits. Many organizations talk of social concern and the fact that they would not want to see their employees be without insurance protection or suffer in their retirement. The major overall aim of benefits from the employer's standpoint is membership, but some other advantages can occur from granting benefits. In order for employees to concentrate on performing well, they must be able to concentrate upon their job. Having protection from uncertainty provides an ability to concentrate. Benefits provide security in three areas: age, unemployment, and health (sickness or accident).
But security is an after-the-fact type of protection. There are also benefits that employers provide with the expectation that their provision will improve or maintain the current level of performance of the employee. These benefits are largely in the form of time off (which is expected to help the employee recuperate or reduce fatigue on the job), programs to improve the health of the employee, and programs to improve the employee's future worth to the organization, such as educational reimbursement.
Legal requirements
Laws affect benefits in two ways: through requiring the employer to provide the benefit, and by monitoring and directing the way in which the benefit is offered and administered.
First, federal regulations state that employers must provide employees with a series of benefits, as a price of hiring employees. These may or may not be considered benefits by employees, but they are a definite wage cost. These benefits include Social Security, Unemployment Insurance, and Workers' Compensation. All three are based upon laws passed decades ago, but changes both in the law and in society make them problematic today. This chapter begins with a discussion of these required benefits.
Second, other laws regulate the way benefits are offered and administered. Employers are not required to offer these benefits but when they do certain laws apply to the way they are structured. ERISA is probably the best example, but many tax laws and codes apply to benefits. These laws will be discussed as the benefit to which they apply is covered.
Contributions and Cost
The costs of providing a benefit are a major consideration. Most benefit administrators can show that the benefits are cost-effective by the savings that they can attain through proper administration of the particular benefits.
Consideration must be given to who should pay for the benefits, or more likely, how much each partner to the employment exchange should contribute to the cost of the benefit. To the degree that the employee pays for the benefit, the employer cannot claim it as their contribution to the employment exchange. There are good reasons to share the costs of particular benefits. The employee sees the benefit more clearly as a part of the employment exchange when costs are shared, and the employee has a larger and more direct stake in keeping benefit costs down when both parties are contributing to the cost of the benefit.
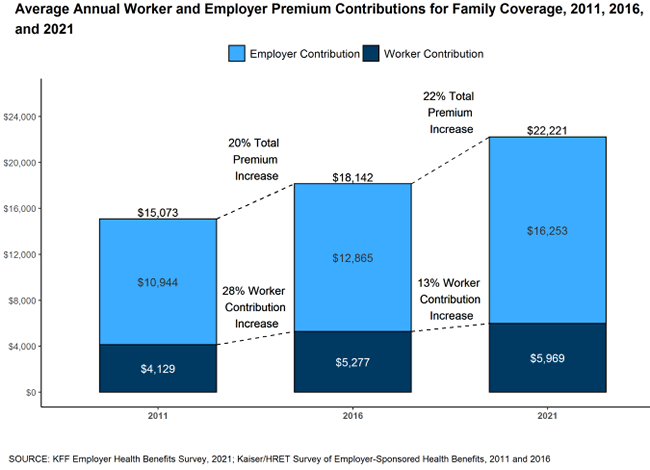
Overall, the cost of benefits has risen substantially year after year. The main force behind this has been the rise in the cost of health benefits, as illustrated in figure 21-1.
TYPES OF BENEFITS
Although there is no set way of classifying benefits, ERI has been surveying and reporting on benefits for many years and uses the five categories of benefits shown in Figure 2.
Type of Benefit
-
Legally required payments (employer's share only)
- Old-age, survivors, disability, and health insurance (FICA taxes)
- Unemployment compensation
- Workers' Compensation (including estimated cost of self-insured)
- Railroad retirement tax, railroad unemployment and cash sickness insurance, state sickness benefits insurance, etc.
-
Retirement plan, insurance, and other agreed-upon payments (employer's share only)
- Retirement plan premiums and retirement plan payments not covered by insurance-type plan (net)
- Life insurance premiums; death benefits; hospital, surgical, medical, and major medical insurance premiums, vision, dental, etc. (net)
- Salary continuation or long-term disability
- Dental insurance premiums
- Discounts on goods and services purchased from company by employees
- Employee meals furnished by company
- Miscellaneous payments (compensation payments in excess of legal requirements, separation or termination pay allowances, moving expenses, etc.)
- Paid rest periods, lunch periods, wash-up time, travel time, clothes-change time, get-ready time, etc.
-
Payments for time not worked
- Paid vacations and payments in lieu of vacation
- Payments for holidays not worked
- Paid sick leave
- Payments for National Guard (or army or other reserve duty); jury, witness, and voting pay allowances; payments for time lost due to death in family or other personal reasons, etc.
-
Other items
- Profit-sharing payments
- Contributions to employee thrift plans
- Christmas or other special bonuses, service awards, suggestion awards, etc.
- Employee education expenditures (tuition refunds, etc.)
- Special wage payments ordered by courts, payments to union stewards, etc.
- Employee assistance programs (drug recovery, alcohol, etc.)
- Gainsharing
Source: Reprinted from Employee Benefits 1984, Copyright 1986 by The Chamber of Commerce of the United States of America. Used by permission of the publisher.
This breakdown will be used as we discuss the major features of today's benefit packages. Some of the benefits (profit sharing and service awards) are awarded for people's performance and not for their membership. As such we considered them elsewhere in this text.
LEGALLY REQUIRED BENEFITS
This section covers the benefits that are required by law, specifically social security, unemployment insurance and workers compensation. The laws these benefits are based upon were developed during the great depression of the 1930's and have undergone many changes over the years.
Social Security
Social Security benefits are based upon the Social Security Act of 1935. Social Security's original intent was to encourage workers to retire at the age of 65 by providing payments to them. At the time of the Depression this was done to attempt to remove these people from the work force and thereby lower unemployment. Social Security currently taxes workers and employers to pay for former workers who have left the work force. In this regard it is a tax system, not a retirement plan.2
Coverage. Over the years Social Security coverage has changed. Old-Age, Survivor and Disability Insurance (OASDI) Social Security covers old-age benefits, aid to dependents and survivors, death benefits and disability benefits. Through the Medicare program Social Security provides medical insurance to people at age 65. As with most such laws, the proportion of the work force covered has also expanded over time.3 In order to pay for this expansion and inflation, the tax has gone up over the years. In 2000, only the first $76,200 in earnings was taxed. In 2022 it rose to $147,000.
Year 2022 FICA and OASDI tax rates are shown below:
| Federal Insurance Contributions Act (FICA) – Medicare | |
|---|---|
| Employee | 1.45% on all wages |
| Employer | 1.45% on all wages |
| Self-employed | 2.9% on net earnings |
| Old Age, Survivors, and Disability Insurance (OASDI) | |
|---|---|
| Employee | 6.2% on first $147,000 of wages |
| Employer | 6.2% on first $147,000 of wages |
| Self-employed | 12.4% on first $147,000 of earnings |
Benefits. The benefits for employees and others from Social Security fall into five categories:
- Old age and Disability payments
- Payments to dependents of retired or disabled employees
- Survivor benefits
- Lump-sum death benefit
- Medicare Part A and B
To qualify employees must have contributed to social Security for 40 quarters. The amount will vary with both years and amount of contribution.4
Problems. The Social Security program encountered problems in the early 1980s. Expenses have risen faster than the income to the program. Indeed, the combination of asking the program to do more than it started out to do, the U.S. population's increasing longevity, the tying of benefit levels to the Consumer Price Index, and the decline in the proportion of the population paying into Social Security, has led to a projected deficit in the program.5 A number of amendments to the Social Security Act made in the 1980s and 1990s purportedly solved the financial problem for 75 years, but as it stands today, Social Security benefit payments exceed the taxes collected to pay for the program, and the trust funds will be empty by 2035.6 Social Security will then be able to pay only about 80% of benefits.
In the past there was a feeling among many employees that Social Security would take care of retirement, so further saving was unnecessary. Likewise, among employers there was the development of retirement plan programs without any consideration of Social Security. The crisis in Social Security provides an opportunity to coordinate Social Security, employer retirement programs, and employee savings programs to provide realistic protection for employees during retirement.
Unemployment Insurance
Protection against loss of income from losing one's job was another protection included in the Social Security Act of 1935. The administration of this program, however, is separate from that of Social Security, being a combination of state and federal administration.
Financing. Unlike Social Security, unemployment insurance is entirely paid for in most states by employer contributions, making it much less visible to the employee. The Federal tax (FUTA) to pay for this benefit is 6.0% of the first $7,000 of the employer’s taxable wages. Of this amount, a certain percent goes to the states for operating their unemployment insurance and job service programs, and the remaining amount or percent goes to the federal government. Employers must pay the tax if they employ one or more individuals in each of twenty different weeks in a calendar year or pay wages of $1,500 or more during any quarter in of a calendar year. The FUTA rate is 6.0 %, but employers are entitled to a credit of up to 5.4% if they pay their state unemployment taxes on time. This makes the net effective FUTA rate for most employers 0.6% or $42.00 per employee. In addition to FUTA, the employer must pay the applicable state tax, which varies by state. For information on these rates go to: http://workforcesecurity.doleta.gov/unemploy/statelaws.asp#sigprouilaws.
Coverage and Eligibility. Unemployment benefits are intended to be available to employees who become unemployed through no fault of their own. All workers are covered by the provisions except for some agricultural and domestic workers. However, in order to be eligible upon becoming unemployed a worker must:
- be able, available, and seeking work
- not have refused suitable work
- not be unemployed because of a labor dispute (there are exceptions to this)
- not have left the job voluntarily
- not have been terminated for gross misconduct
- have been employed in a covered industry, and earned a designated minimum amount for a certain period of time
These requirements reduce the segment eligible for unemployment insurance substantially.7
Benefits. An unemployed worker who qualifies under these requirements is entitled to 26 weeks of unemployment payments in most states. These payments were supposed to be half of the person's lost wages. In fact, benefits are based on a percentage of an individual's earnings over a recent 52-week period - up to a State maximum amount. However, it can feel like more, since these payments are not taxable. During periods of high unemployment, the government often extends the payment period beyond the 26 weeks. For more information, see the Office for Workforce Security at workforcesecurity.doleta.gov
Cost Control. Employers are experience-rated. That is, ex-workers who apply and are granted unemployment benefits are charged against the employer. This increases the cost of unemployment insurance to the employer, so it is in the organization's best interest to see that claims for unemployment are legitimate. A further and more positive approach is to reduce terminations within the organization. The total cost of terminating people is quite high, and programs of intervention before termination are necessary and worthwhile. Also, it is important that production methods and practices that encourage alternating hiring and layoffs of personnel be examined, and that their full costs be made apparent to management.
Employee Motivation. A final concern about unemployment insurance is its effect on the will to work. All of us are aware of or have heard about people who really are not trying to seek work while collecting unemployment insurance. Empirical studies do show that those workers covered by unemployment insurance do remain unemployed for a somewhat longer period. In fact, the law may well have the intended effect of keeping low-level and entry-level positions unattractive to highly skilled and experienced workers and allowing new entrants into the work force even when unemployment is high.8 This allows unemployed workers to improve their labor-market status while unemployed by increasing their education and training. The small disincentive effect of unemployment insurance is offset by its value as worker protection in our industrialized world.
Workers Compensation
Workers' Compensation is a program that provides benefits for employees injured on the job. It is based on state laws, so the requirements vary considerably from state to state.
Legal Requirements. Workers Compensation laws require that covered employers provide insurance to pay for expenses resulting from work-related accidents, injury, or disease. There is no determination of fault in Workers' Compensation. The employer pays fully for this insurance coverage. The insurance is carried through private carriers or in some cases the states themselves. Some states provide a second injury fund to protect a present employer from paying for a previously covered injury. Being a state program, the requirements differ somewhat depending upon the state[s] in which the organization operates.
Workers' Compensation also requires employers to have medical facilities available in case of injury on the job. This has been one of the more successful aspects of the program. However, the part of the law that seeks to reduce accidents through reporting and study has not been nearly as effective.
Coverage. Injured employees are covered both for the costs of the injury and for the time lost off the job. In this regard Workers' Compensation is a combination of medical insurance and disability insurance. The injured employee typically receives 50-67 percent of lost income. Injury and permanent-disability payments are usually paid out on a schedule.
Employer Concerns. The cost of Workers' Compensation is a major concern of the employer. This type of insurance is experience-rated, so it pays for the employer to keep the number of injuries to a minimum. Where this is done through safety programs and education, all parties benefit. However, all injuries must be reported and dealt with to their conclusion.
Of recent concern has been the broadening of the definition of what constitutes a work-related injury or disease. Where the injury is clearly physical and the cause and effect immediate, there is little problem. Complications arise with claims for mental and emotional injury, as well as claims in which the time lag may be several years from the incident to the disease, and these claims are on the rise.9
DISCRETIONARY BENEFITS
Beyond those benefits legally required is a group of benefits that employers offer for reasons other than they are required to do so. This is mostly because of competition for labor and/or the desires of employees. The benefits covered in this section include retirement programs, insurance plans, payment for time not worked and services.
Retirement Programs
This category of benefits, and the next (insurance), validates the statement that in the United States, employee protection arrangements have been left to organizations rather than government. The programs covered in this section are controlled by laws when offered but are not required by law.
Retirement Overview. A major benefit consideration is to provide economic security for employees upon retirement. This can be accomplished in a number of ways. In essence, all methods of providing economic stability in later life are done by deferring current compensation to some future time, but some programs do this more obviously than others. The least visible form to the employee is the retirement plan program. In a retirement plan program, money is put away in a fund each year for the employee's eventual retirement. At retirement the employee begins to receive the money put away for him or her. Thus, a retirement plan program is a trade-off between current income and future security. It is not strange, then, that desire for, and interest in, retirement plan programs increase with age. The problem is that in order to have a retirement income that is satisfactory, one must take an active part from a young age.
Retirement plan programs have been a part of organization benefit packages for a long time. During the early 1970s there was a great deal of concern about retirement plan programs as it became clear that many employees who thought they were covered by such programs discovered that they were not. This was partially an administrative situation involving very complicated plans. It was also an economic problem where organizations had not funded their pension plans and could not meet the demands of retirees. The result of these problems was the Employee Retirement Income Security Act (ERISA), which sets forth the standards that the organization's retirement plan program must meet. The act does not say that the organization must have a retirement plan program, but does say that if it does have a retirement plan program, that program must meet certain standards.10
In addition to ERISA, tax laws affect the development and administration of retirement plan programs. Since there is a deferral of income from today to tomorrow, the IRS is interested in seeing that this deferral is not abused to avoid taxation. In addition, the tax laws are concerned with treating all employees in the organization in a nondiscriminatory manner. What this means is that retirement plans cannot be established that benefit only a portion of the organization's employees, usually executives, if the plan is to qualify for the above-mentioned tax advantages. Again, this does not mean that the organization cannot establish a retirement that does not meet these requirements just that the program will be considered a non-qualified plan that does not have the tax advantages mentioned above. Most such plans are developed for executives. See ERI DLC course 42 — Accumulated Earnings and Deferred Compensation.
The design of a retirement plan program calls for identifying who, when, and how.
Who is in the program?
Our placement of benefits, as membership rewards in the employment exchange, would suggest that a retirement plan program include all employees. But this may ignore two factors: length of time in the organization and the associated value of retaining different groups of employees. If the program is to encourage continued membership, then a waiting period before entrance into the program makes sense. Likewise, certain groups, particularly executives, have needs and expectations that are different from those of other employee groups.
ERISA has some rules regarding who shall be in the program. The law requires that any employee who (1) has been employed for one year or (2) is 21 years of age, whichever occurs later, must be included.
Tax considerations have to do with whether the program is qualified. Participation eligibility must be 70 percent and the participation rate at least 80 percent of the eligible population. The importance to the employee of the plan being qualified is that the monies placed in the fund for the employee are not counted as income to the employee in that year. Thus, in order to be qualified, retirement plan programs must benefit only employees and their beneficiaries and not discriminate in favor of particular employee groups, such as executives.
Vesting. A second part of the 'who' question involves the idea of vesting. The term vesting means that the employee has an interest in the accrued benefits of the retirement plan program. In all cases, the employee is entitled to any money that he/she has contributed into the plan. There is a waiting period for the employer's contributions only. Once vested these benefits cannot be taken away even if the employee quits or is, fired. This is a requirement of ERISA and was placed in the law so organizations could not avoid paying retirement plans to employees by letting people go just before their retirement age. Having to stay all of one's working life with a particular organization in order to receive a retirement plan reduces labor mobility drastically, and ERISA allows mobility for the modern career path.
Vesting schedules have been gradually reduced under changes to the law. For 2002 and beyond, the Economic Growth and Tax Relief Act [EGTRRA] requires companies to adopt one of two vesting schedules:
- 3-year cliff vesting: 0% vesting for less than 3 years of service; 100% vesting after 3 years
- 6-year graded vesting: vesting begins in the employees second year of service; it increases by 20% each year, until the employee is fully vested at the beginning of the sixth year of employment
When are benefits paid?
The easy answer to this is when the employee retires. But this answer hides more than it reveals. When is retirement?
Ordinarily retirement plan programs assume a retirement age of 65. The Age Discrimination Act says that employers cannot force a person to retire before 70, and some states have abolished mandatory retirement entirely. Today, there is a trend to postpone retirement past the age of 65.11 Most organizations stay with the 65 figure as a model and adjust the payments made to people who retire early or late actuarially. An alternative way of dealing with this question is to define a number of years of service in the organization before the person is able to obtain full retirement plan benefits.
There are two circumstances other than retirement, in which there is a payout from the retirement plan: death or disability. Upon the employee's death the usual practice is to provide the deceased's beneficiary with the money that is in trust for the deceased. Most pension programs also have a disability retirement clause that, much like an early-retirement provision, pays the employee a proportion of the amount that the employee would be entitled to had he/she stayed employed until the normal retirement date.
How much?
This is the most complex question to answer and one that is affected by at least two major variables. The first of these is the contributor. In some plans only the employer contributes; in others both employer and employee contribute. Employee contribution plans tend to pay more than noncontributory ones. On top of Social Security, a further deduction from the paycheck may seem like a lot to the employee and certainly reduces his or her options for putting money away in other ways. But it also makes the retirement plan program more visible to the employee and makes it a shared contribution to the employment exchange.
The second variable is the type of program: defined benefit or defined contribution. These are so different that they are discussed separately below.
Defined-benefit plans. A defined-benefit plan is one in which the employee, upon retirement, is guaranteed a set income for as long as he or she lives. There is usually a clause that also allows a percentage continuance beyond death, for the person's spouse. This used to be the most common form of retirement plan program. The exact benefit amount is determined by the employee's income and the number of years of service, with age as another variable. The current wage rate, or an average of the wage rate for a previous time period, forms the base for determining the amount to be paid.12
The length of service determines the percentage of the base pay that will be paid out each month. This figure is ordinarily some small percentage per year, from 1 to 5 percent. An employee with 30 years of service and a 3 percent accrual per year is entitled to 90 percent of base pay. This percentage need not be the same each year. A front-loaded program gives a person a higher percentage in the early years of coverage and a lower percentage in later years. A back-loaded program does just the opposite. The two have very different consequences for employee retirement decisions. A front-loaded plan makes early retirement attractive, since additional years do not add much to the person's retirement income. A back-loaded program makes staying on the job to the normal retirement time more attractive, since it is the last few years that make a large difference in retirement income.
Under ERISA the employer must contribute to the retirement plan fund, enough monies each year, to fund the additional value that the employee has gained in the retirement plan program. In a defined benefit plan, there is a problem in determining what this amount should be. It is a complex actuarial decision that must be made by an expert.
Three other considerations with defined benefit plans need to be discussed. The first is the effect of inflation. If the plan provides a certain income at retirement without a way of adjusting for inflation, the value of the retirement plan can decline rapidly after retirement. This is very difficult for the former employee who has planned on a reasonable retirement program and finds it is inadequate. On the other hand, automatic adjustments tied to the CPI can break the program; so, most retirement plan programs are granting ad hoc increases as deemed necessary.
A second consideration is male-female discrimination. Women live longer, so there have been attempts over the years to either lower the payment amounts to women, or to make women contribute more to the program. Both alternatives have been ruled out by the Supreme Court, so retirement plan programs may make no distinction because of gender.
The third consideration is the possibility of integrating the retirement plan program with Social Security. This can be a cost-cutting strategy for the organization since benefit levels can be lowered if Social Security benefits are taken into account in determining the benefit levels that are appropriate for the organization's employees. There are two methods of integration. The first, an offset approach, subtracts a particular fraction of the qualified pension plan benefit from the total benefit without integration. The second, an excess approach, stipulates a compensation amount known as the integration level.13
Defined-contribution plans
In a defined-contribution plan, employees do not know what income they will receive upon retirement but do know how much money there is in the retirement plan fund earmarked for them. Upon retirement the person can take that money out and develop a retirement-income program.
The money in the defined-contribution plan may come from the employer, the employee, or a combination of both, as well as the interest earned on those contributions. The employer contributions can be determined in a number of ways. The easiest is a percentage of the person's pay each year. More complex, but of more interest to many organizations, is the combination of a defined-contribution plan with a profit-sharing program.
Defined-contribution plans are now far more numerous than defined-benefit plans and are growing at a faster rate. Part of the reason is their comparative simplicity. The employer contribution is much easier to calculate and understand under a defined-contribution plan.
401(k) plans. Social Security's funding problems and the dramatic inflation rates of the late 1970s led to the realization that employees must plan for their own future retirement and not depend upon the government to take care of them. This trend toward independence has been encouraged by the government; they have established a number of programs to allow individuals to invest money and defer the taxes on that money until retirement.
401(k) plans are the best example of this trend. They are a defined contribution plan, that if properly administered and sold to the employees, is a qualified plan under the tax laws. A 401(k) plan allows the employee to put aside up to the following:
| Maximum Limits |
|---|
| 2022 . . . $20,500 |
In addition, the Economic Growth and Tax Relief Reconciliation Act of 2001 offers employees over 50 a "catch-up" provision, which lets them contribute an extra $6,500.
The organization may provide matching funds if it wishes. This matching can be one for one, some percentage, or tied to profits. The most common matching is 50% of the employee's contribution. The limit for contributions (employee, employer, and any reallocated forfeitures) allocated to a participant's account for any year is the lesser of 100% of compensation or $61,000, or $67,500 with the catch-up provision (2022).
The monies collected may go into a single fund or may be allocated among a number of funds by the employee. If multiple funds have been chosen, the employee can switch funds as needed. These plans may also have a loan program that allows the employee to take money out for emergencies. Discrimination tests make it imperative that considerable thought and communication be implemented when managing a 401(k); participants must include all levels of employees in the organization and not just the executives and higher paid employees. Despite these requirements, 401(k) plans are the fastest-growing retirement plan benefit today.14
Profit-Sharing Plans. A profit-sharing plan may be considered a defined contribution plan if the distributions are placed in individual employee accounts and deferred until retirement. A profit-sharing plan is established by the organization setting aside some proportion of profits to be distributed to the employees. This pot of money is distributed, using a formula, into the individual employee accounts. For a more comprehensive discussion of profit-sharing plans see Chapter 18 of this text or ERIDLC course 75-Creating an Incentive Pay Plan.
Another type of plan, similar to profit-sharing, is a Stock Bonus Plan. In this plan, employees are granted stock of the company that is held until retirement. This type of plan might bring greater loyalty to the organization, but it puts the retirement fund in jeopardy if the fortunes of the company decline.
ESOPs. Employee stock ownership plans (ESOPs) are also a form of defined-contribution program. The idea of these plans is that the employer puts money aside for the employee, which is used to purchase stock in the company. These ESOPs are attractive to organizations because they can borrow money to purchase the stock and pay off the loan and interest with taxable income. Banks are permitted to exclude 50 percent of interest on ESOP loan value from taxable income. If the company does well, these plans are seen positively by employees, but if the company does not do well the employee receives little value. Again, employee stock-ownership plans are also a form of defined-contribution program, one that has been used for non-retirement objectives. Common to these plans is the ability to borrow money and have the employees purchase all the stock of the company).15 Often, these plans are used in an attempt to rescue a dying company; individuals' retirement monies are used to support what otherwise no one would buy. (Employees purchase the company or "buy a job" with their retirement savings.) The track record of ESOPs from a financial perspective is mixed.16
SEPS, SIMPLEs and IRAs. A new form of retirement program allowed by law is the simplified employee retirement plan (SEP). This is a form of individual retirement account (IRA) in which the employer is allowed to contribute a percent of the employee's income into a savings account. This is a popular form of retirement plan program because it requires little administration. It is particularly valuable to small organizations.17
A Savings Incentive Match Plan for Employees [SIMPLE] is like a SEP but both the employer and employee can contribute to it. The retirement plan may take the form of an IRA or a 401k.18
Individual Retirement Accounts (IRAs) allow individuals to contribute funds on their own without the assistance of a company sponsored plan. Any U.S. taxpayer who works, whether as an employee or self-employed, can set aside up to $6,000 per year in an IRA, or $7,000 for persons over 50 (2022). The earnings on these investments grow, tax-deferred, until the eventual date of distribution. Individuals may also set up Roth IRAs, to which contributions are not deductible, but from which withdrawals at retirement won't be taxed.
INSURANCE PROGRAMS
Organizations typically offer insurance benefits for employees in three categories: 1) health and medical, 2) disability and 3) life. There are two major benefits from having the organization provide this insurance, as opposed to having the employees obtain it themselves: taxability and group rates. As a benefit, payments made by the employer for the insurance are not considered to be income to the employee. The employer acting as a representative of the group of employees can obtain a better rate for all employees by putting them into a group program. This is a very real advantage and one that will continue to be effective.
One consideration that runs through all these types of insurance programs is the question of employee contribution. Traditionally, medical programs have been paid for by the employer, life insurance is split between employer and employee, and disability is usually paid for by the employee. More and more, employers are asking employees to contribute to the cost of Medical Insurance as described in Chapter 20.
When the employee pays for all or some of the cost of the insurance, the value of the benefit in the employment exchange goes down, but the attention that the employee gives to the benefit goes up. In today's families where both spouses are employed, there also exists the probability that both have family coverage for the same type of insurances. It makes sense to the employee with the lowest cost/best benefits plan to have everyone in the family on the plan, including the other working spouse. This is not, however, desirable for the employer and they may ask their employees to pay disproportionately more if the spouse is included in the plan.
Health/Medical Programs
The purpose of health insurance programs is to provide protection from the costs, sometimes enormous, of sickness and accident to employee and their families. This is done in two ways: an insurance plan or a health maintenance organization (HMO).
Insurance Plans
Insurance plans are fee-for-service plans in which the organization contracts with an insurance company to provide the plan, called an indemnity plan. The organization may choose to self-fund the plan, but the plan will still be a fee-for-service plan. In fact, many organizations that self-insure hire an insurance company to administer the plan. Indemnity plans come in a number of forms to be discussed here:
- Traditional plans
- Major Medical Plans
- Preferred Provider Plans (PPO)
- Point-of-Service Plans
- High Deductible Health Plans (HDHP)
Traditional Plans. These programs collect money from the employer into a fund and pay it out as employees and their families have health needs. Employees put in claims, usually to the insurance company, when they incur medical expenses. Blue Cross and Blue Shield come to mind as representative of this type of plan. The amount that the employer puts into the fund must, over time, equal the claims against the fund plus the administrative costs of operating the fund. Rates go up when this does not happen. The program must define the health charges that will be accepted for payment and determine what proportion of the costs the insurance program will cover. As an alternative, the program determines the amount that will be paid for any particular service.
Some organizations choose to self-insure. This means that the organization provides the agreed-upon coverage to employees out of its own assets instead of turning over a sum of money to the insurance company. This has been a way in which organizations have been able to reduce their health insurance costs. Of course, in doing so they are moving the risk from the insurance company to themselves.
Major medical Plans. These plans are like the traditional plan, however, they contain a high deductible so the employee would have to incur a high (say $5,000) medical bill before this plan would protect them. The advantage of these plans is they have much lower premiums. Employers often use these types of plans as a supplement to traditional plans and they take effect after maximums have been reached.
Preferred Provider Organizations. PPOs are organizations that contract with a group of doctors and hospitals to provide services at a discounted price. The PPO establishes standards for the providers and sets reimbursement levels. These plans usually have co-pays and a deductible for the year, per covered person, and pay a percentage, 80% to 100% of the costs depending on the care provided. This is attractive to the providers because it produces a consistent flow of patients. The PPO is halfway between a regular insurance plan and an HMO. The employee is free to go to any doctor or facility on the list.19
Point-of-Service Plans. Like a PPO, POS plans have a network of health care providers that the employee should use and there is a co-pay but usually no deductible for the use of these providers. The employee may go outside the network but pays more for this privilege.20
High Deductible Health Plan. These plans have higher deductibles and correspondingly lower premiums than typical health plans requiring employees to pay more out-of-pocket. HDHPs are often offered with a Health Savings Account (HSA) that lets the employee put aside money pre-tax to pay for qualified medical expenses. Withdrawals to pay medical expenses are tax-free.
There are different types of HSAs. A Medical Savings Account is a tax-exempt trust or custodial account set up with a U.S. financial institution (such as a bank or an insurance company) into which the employee can save money exclusively for future medical expenses. This type of plan is used for self-employed persons or those working in small organizations. A Flexible Spending Arrangement (FSA) allows employees to be reimbursed for medical expenses. FSAs are usually funded through voluntary salary reduction agreements with the employer. No employment or federal income taxes are deducted from the contributions. The employer may also contribute. A Health Reimbursement Arrangement (HRA) must be funded solely by the employer. The contribution cannot be paid through a voluntary salary reduction agreement on the part of the employee. Employees are reimbursed tax free for qualified medical expenses up to a maximum dollar amount for a coverage period. An HRA may be offered with other health plans, including FSAs.21
Health Maintenance Organizations (HMOs)
An HMO is an organization that combines being an insurance company and providing health care. It offers comprehensive health care, both inpatient and outpatient but on a pre-paid basis; all services are provided at a fixed fee. HMOs are supposed to focus on preventive medicine as well as taking care of current health problems. The Health Maintenance Act of 1973 sought to encourage the use of HMO's by making it a requirement to offer an HMO option if the organization is subject to the minimum wage provisions of the Fair Labor Standards Act. HMOs vary greatly in their success but over time have been attracting a larger share of the health care market. They differ considerably from the traditional insurance plan in that they use capitation instead of fee-for-service. That is there is an exchange of the money for complete care as opposed for paying for each medical event.
Other health-related insurance
Most health insurance plans limit the area of health covered. In particular, dental and eye care are usually excluded and covered under separate policies. Sometimes, pharmaceuticals are also covered in separate programs.
Health care coverage
Health care programs usually cover all employees. However, many organizations exclude part-time employees from coverage. In some cases, organizations have different plans for different employee groups; managers and executives often have plans that include wider coverage.
The Consolidated Omnibus Reconciliation Act of 1985 (COBRA) requires that employees, their spouses, and their children must be offered medical coverage after the employee is no longer employed by the organization. The coverage is for 18-36 months, depending on the circumstances. The employer is allowed to charge the covered person 103 percent of the premium cost. (COBRA can vary among employee groups as some states have passed their own COBRA supplements.)
Containment of Health Care Costs
Health care is a good example of a benefit that has gone out of control. When organizations first started offering health insurance it was cheap and health-care costs were relatively low. In addition, organizations began offering the benefit in terms of coverage and not in terms of cost. Then came the dramatic increase in the costs of health care. In 1960 the proportion of GDP devoted to health care was 5 percent. By 2000 it had grown to 13.3 percent and in 2022 it stood at 19.7 percent. The cost of health-care coverage to the organization has likewise risen as organizations agreed to provide health care coverage regardless of cost. At this point organizations have started looking toward ways of controlling health-care costs. Some of these alternatives have already been mentioned: HMOs and self-insuring were some of the first to appear.
Probably the most successful technique in cost containment is sharing the cost with the employee. This can be done at two points. The first is to share the premium costs of the insurance. The second is to share the health-care charges. This can be done by having deductibles for overall service or for specific services. This may take place informally in nonunion organizations or as a part of collective bargaining in unionized organizations.
Close administration of health-care programs is also necessary. Knowing who is being paid and for what can lead to identification of abuses in the system. Claims control is important, allowing administrators to see that the providers are charging correctly and that employees are properly making claims on the program. Communication and education can alert the employee to the costs the employer must put into this area and therefore not into others. Further, educational efforts directed at promoting health, reduce claims and provide a better-performing employee.22
Disability Insurance
Workers' Compensation (discussed above) takes care of a disability resulting from injury on the job, and health insurance takes care of the medical costs of non-work-related injuries. But a person who is out of work because of a non-work-related injury or illness faces a loss of income at the very time that it is important to have full income. Disability insurance is designed to fill this need. Several states (and Puerto Rico) have a legal requirement for disability protection for the employee.
The immediate form of disability coverage is sick leave. This is not really insurance but payment for time not worked. But the effect is the same: the employee's salary is continued while he or she is ill. From the organization's standpoint it is like self-insurance.
Long-term disability is taken care of by an insurance program that specifically pays a proportion of the employee's salary for a specified period. This is commonly an option employees may choose if they are willing to pay for it. (If a company pays for this benefit, then any benefits paid are taxable. If the employee pays, then the benefits are non-taxable.)23
Life Insurance
Life insurance is one of the most common benefits offered by organizations. The insurance is usually of the group-term type, which provides coverage for a certain period with no cash surrender value or investment value. The amount of coverage is geared to the salary rate of the employee: the higher the salary the more insurance the employee is allowed.
Organizations vary as to whether the premiums for this insurance are paid by the employee or by the organization. When these benefits are paid for by an employer, coverages above certain amounts create imputed income that is shown on an employee's W-2 each year.
DISCRIMINATION TESTS
Misunderstood by many is the fact that certain benefit coverages are required to pass discrimination tests. Should they not pass these tests, then the benefits are classified as wages/salaries and the employees are taxed. Examples include: self funded medical plans (Tax Code Section 105(h)), life insurance (S79), and cafeteria plans (S125).
DIFFERENCES IN BENEFITS
During the 1990s, various states began to accelerate the adoption of compensation and benefit laws that were more favorable than federal laws. In the wage and salary area, minimum wage laws are an example. Many states have mandated rates higher than the federal minimum wage. However, with retirement benefits, this has not been the case. ERISA has been upheld numerous times in the Courts as superseding state laws.
There is a sound reason for this. If every state had its own laws governing retirement plans, then any organization operating across state boundaries could find itself violating one state's laws by meeting another's. This ability to operate across state boundaries has been critical to the growth of the American economy. (Canada operates under the opposite principal: federal law should not supersede Provincial. This has been detrimental to their businesses.)
However, the Health Insurance Portability and Accountability Act of 1996 (HIPAA) does allow states to pass laws superseding federal regulations. Since 1974, U.S. federal law has been firmly established related to welfare and retirement benefits. States are not allowed to pass laws that supersede ERISA. For medical benefits and insurance, that feature (which allowed companies to easily operate across state boundaries) has now been amended by HIPAA so that states that pass laws that are more favorable to employees related to medical benefits have the right to supersede federal law.
Chiropractic Coverage
Chiropractic care is available to members of the armed forces at more than 40 military bases in the U.S., and at nearly 30 veteran's administration medical facilities. The U.S. Congress has authorized that certain chiropractic services for all Americans be covered by Medicare and Medicaid. Federal employees have chiropractic coverage in the Federal Employee Health Benefit Program and in the Federal Employee Worker's Compensation Program. Chiropractic treatment is a covered benefit in virtually all traditional insurance policies. In fact, according to some reports, as many as 87 percent of all insured American workers have coverage for chiropractic services in their health care plans. All 50 states have authorized the provision of chiropractic care under state workers' compensation laws. Chiropractic services are included in the Railroad Retirement Act. The Internal Revenue Service includes chiropractic services as a valid medical deduction.
PAYMENT FOR TIME NOT WORKED
This category of benefits includes a number of situations in which the employee is paid but is not actually working. It can include both time at the workplace and time away from the workplace.
Time Not Worked on the Job
Included in this category of benefits are arrangements for rest periods, lunch breaks, and various preparatory activities and cleanup activities at the end of the day. Most of these arrangements have come about historically and are informal. In some cases, they are predicated on state laws (see wage and hour laws), requiring breaks after a certain work time or negotiated as part of a labor contract.
Time Off the Job
This is a category of benefits that many employees have come to expect: vacations, holidays, sick leave, maternity leave and personal leave.
Vacation
The purpose of vacation is to give the employee time away from the job for rest and recreation. Over time there has been a trend toward granting more vacation time. This trend, if not being currently reversed, is clearly on hold. The practice seems to be to start with two weeks and work up to four weeks' vacation at 10 to 15 years. Allotting days or hours of vacation may be done on a yearly basis or upon the number of hours worked.
The major issues in vacation policies are:
- Who is eligible? This question revolves around new employees and part-time employees
- Scheduling vacations so as not to disturb workflow
- Whether vacation time can be carried over, and if so, how much
- Can the employee "cash out" unused vacation time
- Whether to give a payout to the employee if the vacation time is forfeited.
Allowing employees to build up a bank of vacation time creates a large potential cost to the organization and destroys the purpose of vacation – to get away from the job, so most companies have a policy limiting the amount of vacation time that can be carried over.
Holidays
The common number of paid holidays per year ranges from 8 to 11; the latter is the number of days granted federal employees. Some of these are legally defined and others are the product of tradition or bargaining. Upturns in the economy and concession bargaining have in the past increased the number of holidays in many industries.
Sick leave
The most common amount of sick leave is one day a month, amounting to 12 days a year. There are two opposing concerns with sick leave. The first is the person who abuses sick leave by taking it whether really sick or not. This employee then has no sick leave available when it is needed. The opposite problem is those employees who take no sick leave and thereby build up a large potential cost to the organization. This can be quite costly, since employees could build up their reserve while their salary rate is low and then use it when their salary rate is much higher. Every time the wage structure is adjusted, this affects the total potential cost of sick leave. To get around this problem organizations are limiting the buildup of sick leave just as they are vacations.
Maternity leave
Employer provision of maternity health care benefits play an important role in a benefit plan, especially as more and more women of childbearing age participate in the workforce. Most company-sponsored health care plans provide for prenatal care, delivery, and postnatal care.
The Family and Medical Leave Act of 1993 [FMLA] requires that a leave of absence, up to 12 workweeks, be granted to any employee for:
- Birth and care of a newborn child
- Adoption
- Care of an immediate family member with a serious illness
- Medical leave when the employee is unable to work because of a serious health condition.
This leave does not have to be paid leave but the employee is entitled to return to their job or an equivalent one.
Personal leave
This is a grab bag of time off for various reasons, such as a death in the family, military leave, and jury duty. Many organizations are setting up a general category of personal leave rather than having a series of special circumstances that lead to different interpretations throughout the organization. In fact, many organizations now combine personal leave, vacation, and sick leave into personal time off or PTO. It is left up to the employee to decide how these days are to be distributed.
REPORTING
Benefits plans are required to be reported to both the government and the plan participants. The Internet has brought changes to this laborious process, particularly with the acceptance of e-signatures for all benefit plans. See Chapter 26 for further discussion of this issue.
EMPLOYEE SERVICES
A number of other benefits are often granted to employees because they are of value to the employee. While not of great value to the employer, it is the employer who can arrange for the service, grouping employees to provide an economic advantage in dealing with the suppliers of the service, much as is done in insurance. Examples of this are credit unions, food services, recreational facilities, and discount tickets to entertainment events.
These services are appreciated by the employee and also enhance the value of the employee to the organization at the same time. The three best examples of this are reimbursement for educational expenses, health-club or recreational-club memberships, and day care for children. In each of these cases, the employer is spending money to provide the employee with a service that will improve the ability of employees to accomplish their job.
Educational Expense Reimbursement
This has been popular for a long time, particularly among professional and managerial employees who are seeking advanced degrees. The organization ordinarily pays the tuition of the employee, provided the educational experience relates to the job. In addition, adjustment of the working day is often required to allow part-time students to attend classes.
Health-Club Memberships
The development of a health facility on plant premises is increasing with the knowledge that a healthy person is a more productive employee. The movement toward concern with health in the United States has spurred this trend. Many organizations claim that this, plus a campaign to promote wellness among employees, reduces absenteeism, increases productivity, and lowers medical-insurance costs.
Family Assistance Programs
In this era of people caught in between their children and their aging parents, there is a need for help from the employing organization to understand and help employees caught in this squeeze. Finding proper facilities to take care of children and ill or ageing parents is difficult. Organizations have found it helpful to at least search out referral sources that can be provided to employees.
Some organizations choose to go further than just referrals. Sponsoring or underwriting elder or child care facilities is one option. Another is to actually set up a child care facility on or near the organization's facility.
SUMMARY
Benefits represent a wide variety of rewards granted to employees for a number of reasons. Each benefit requires discussion, since the administration of each is different. Typically, the assortment of benefits is grouped by category and their characteristics are carefully weighed and examined.
Legally required benefits include Social Security, unemployment insurance, and Workers' Compensation. All three of these were begun in the Depression era to provide employees with protection against old age, unemployment, and job-related injury. The employer pays part or all of the cost of these benefits. Social Security will have problems in the future if not reformed, as Social Security benefit payments are now greater than taxes collected, and the trust funds will be empty by 2035. Workers' Compensation has been expanding the definition of "job related" to include mental and emotional injury, as well as diseases which develop over time.
The passage of ERISA has made an enormous impact on the design and administration of retirement programs through the requirements for funding, vesting, and reporting. (See: www.dol.gov.) Retirement programs are either defined benefit or defined contribution plans. The has become more popular because of the funding requirements of ERISA. Tax laws have encouraged a number of new types of plans in including 401(k)s and ESOPs.
Another category of benefits is insurance programs. These include health/ medical plans, disability, and life insurance. Medical plans have been the most challenging as costs have risen significantly. A major concern in organizations today is reducing these costs. Some ways of doing this have been the use of HMOs and HDHPs, self-insuring, close administration, and cost sharing with the employee. From a cost perspective, health/ medical plans are the most expensive. Time off work (both paid and unpaid) is an important benefit for maintaining employees' health and wellbeing. These can include vacations, holidays, sick leave, maternity leave and personal leave. The passage of the Family and Medical Leave Act of 1993 granted qualifying employees 12 weeks of unpaid leave per year for special circumstances.
A final category of benefits is employee services, which can include a wide variety of services depending on the organizational circumstance. The current concern in this category is the provision of day care for children of employees.
Footnotes
1 For more information go to: www.ebri.org/
2 www.ssa.gov/history/brief.html
3 www.ssa.gov/policy/docs/statcomps/supplement/2003/highlights.pdf
5 Paine, T. "Alternative Ways to fix Social Security," Benefits Quarterly, Third Quarter, 1997. pp.14-18.
6 "Summary: Actuarial Status of the Social Security Trust Funds," 2022 Annual Report of the Social Security Board of Trustees, Annual Report
8 C. Vickery, "Unemployment Insurance: A Positive Reappraisal," Industrial Relations, Winter 1979, p. 18
9 Lencsis, P.M., Workers Compensation: A Reference and Guide, Westport, Conn. Quorum Books, 1998.
10 Coleman, B. Primer on Employee Retirement Income Security Act 3rd. Ed., Washington, D.C., The Bureau of National Affairs, 1989.
11 For an example see www.pewresearch.org.
12 Martocchio, J.J., Employee Benefits: A Primer for Human Resource Professionals, New York, McGraw-Hill, 2003.
13 Beam, B. & McFadden, Employee Benefits 6th Ed. Chicago, Ill, Dearborn Financial Publishing, 2001.
14 See www.dol.gov
15 Thomsen, D.J., "Calculating the Score on ESOPs", Personnel Administrator, 1975
16 Thomsen, D.J., "Employee Stock Ownership Plans", Personnel Journal, July 1979.
17 See: www.irs.gov
18 www.irs.gov
19 Boland, P. Ed., New Healthcare Market: A guide to PPO's: For Purchasers, Payors and Providers, Aspen Publishers, 1988.
21 www.irs.gov/publications/p969/ar02.html
22 R. M. McCaffery, Managing the Employee Benefits Program Boston, PWS-Kent, 1988
Internet Based Benefits & Compensation Administration
Thomas J. Atchison
David W. Belcher
David J. Thomsen
ERI Economic Research Institute
Copyright © 2000 -
Library of Congress Cataloging-in-Publication Data
HF5549.5.C67B45 1987 658.3'2 86-25494 ISBN 0-13-154790-9
Previously published under the title of Wage and Salary Administration.
The framework for this text was originally copyrighted in 1987, 1974, 1962, and 1955 by Prentice-Hall, Inc. All rights were acquired by ERI in 2000 via reverted rights from the Belcher Scholarship Foundation and Thomas Atchison.
All rights reserved. No part of this text may be reproduced for sale, in any form or by any means, without permission in writing from ERI Economic Research Institute. Students may download and print chapters, graphs, and case studies from this text via an Internet browser for their personal use.
Printed in the United States of America
10 9 8 7 6 5 4 3 2 1
ISBN 0-13-154790-9 01
The ERI Distance Learning Center is registered with the National Association of State Boards of Accountancy (NASBA) as a sponsor of continuing professional education on the National Registry of CPE Sponsors. State boards of accountancy have final authority on the acceptance of individual courses for CPE credit. Complaints regarding registered sponsors may be submitted to the National Registry of CPE Sponsors through its website: www.learningmarket.org.




